Medical Care
Prevalence Rates of Diabetic Retinopathy and Undiagnosed Diabetes Among Delaware Nursing Home and Assisted Living Facility Residents
WHAT THIS MEANS FOR YOU: This cross-sectional study examined eye test data from 2005-2009 in 22 facilities in Delaware to find prevalence of undiagnosed diabetes in assisted living and nursing home residents. A total of 3.6% of residents had hemorrhages in at least one eye, and of these residents, only 56.8% had a diabetes diagnosis, which is connected to eye hemorrhages. The results suggest a need for regular eye care for diabetic and non-diabetic residents to prevent adverse outcomes.
Prevalence Rates of Diabetic Retinopathy and Undiagnosed Diabetes Among Delaware Nursing Home and Assisted Living Facility Residents
WHAT THIS MEANS FOR YOU: This cross-sectional study examined eye test data from 2005-2009 in 22 facilities in Delaware to find prevalence of undiagnosed diabetes in assisted living and nursing home residents. A total of 3.6% of residents had hemorrhages in at least one eye, and of these residents, only 56.8% had a diabetes diagnosis, which is connected to eye hemorrhages. The results suggest a need for regular eye care for diabetic and non-diabetic residents to prevent adverse outcomes.

Be Well in AL Recommendations: Resident/Family Checklist
CEAL@UNC recognizes the benefit of ongoing quality improvement in assisted living, including through the implementation of consensus medical and mental health care recommendations disseminated through the Be Well in AL Initiative. This checklist, to be used by residents and their families considering or residing in assisted living, is a helpful tool to understand recommended care […]
Be Well in AL Recommendations: Resident/Family Checklist
CEAL@UNC recognizes the benefit of ongoing quality improvement in assisted living, including through the implementation of consensus medical and mental health care recommendations disseminated through the Be Well in AL Initiative. This checklist, to be used by residents and their families considering or residing in assisted living, is a helpful tool to understand recommended care […]
The Experiences of Routine Powered Mobility Users in an Assisted Living Facility: A Case Study
WHAT THIS MEANS FOR YOU: A case study of 2 powered mobility device (PMD) users in the same AL community in Ohio used interviews, observational data, and digital image profiling to understand their experiences. The main themes to emerge were initial disapproval of needing a PMD, the actual need for PMD to enable movement, its impact on independence, and training – or a lack thereof – for using the PMD.
The Experiences of Routine Powered Mobility Users in an Assisted Living Facility: A Case Study
WHAT THIS MEANS FOR YOU: A case study of 2 powered mobility device (PMD) users in the same AL community in Ohio used interviews, observational data, and digital image profiling to understand their experiences. The main themes to emerge were initial disapproval of needing a PMD, the actual need for PMD to enable movement, its impact on independence, and training – or a lack thereof – for using the PMD.
Changes in Nursing Staff Levels and Injury-Related Emergency Department Visits among Assisted Living Residents with Alzheimers Disease and Related Dementias
WHAT THIS MEANS FOR YOU: An analysis of 2007-2015 Medicare data for over 12,000 AL residents with ADRD in 455 Ohio AL communities showed that higher levels of RN staffing hours per resident per day led to a 53% decrease in injury-related emergency department visits.
Changes in Nursing Staff Levels and Injury-Related Emergency Department Visits among Assisted Living Residents with Alzheimers Disease and Related Dementias
WHAT THIS MEANS FOR YOU: An analysis of 2007-2015 Medicare data for over 12,000 AL residents with ADRD in 455 Ohio AL communities showed that higher levels of RN staffing hours per resident per day led to a 53% decrease in injury-related emergency department visits.
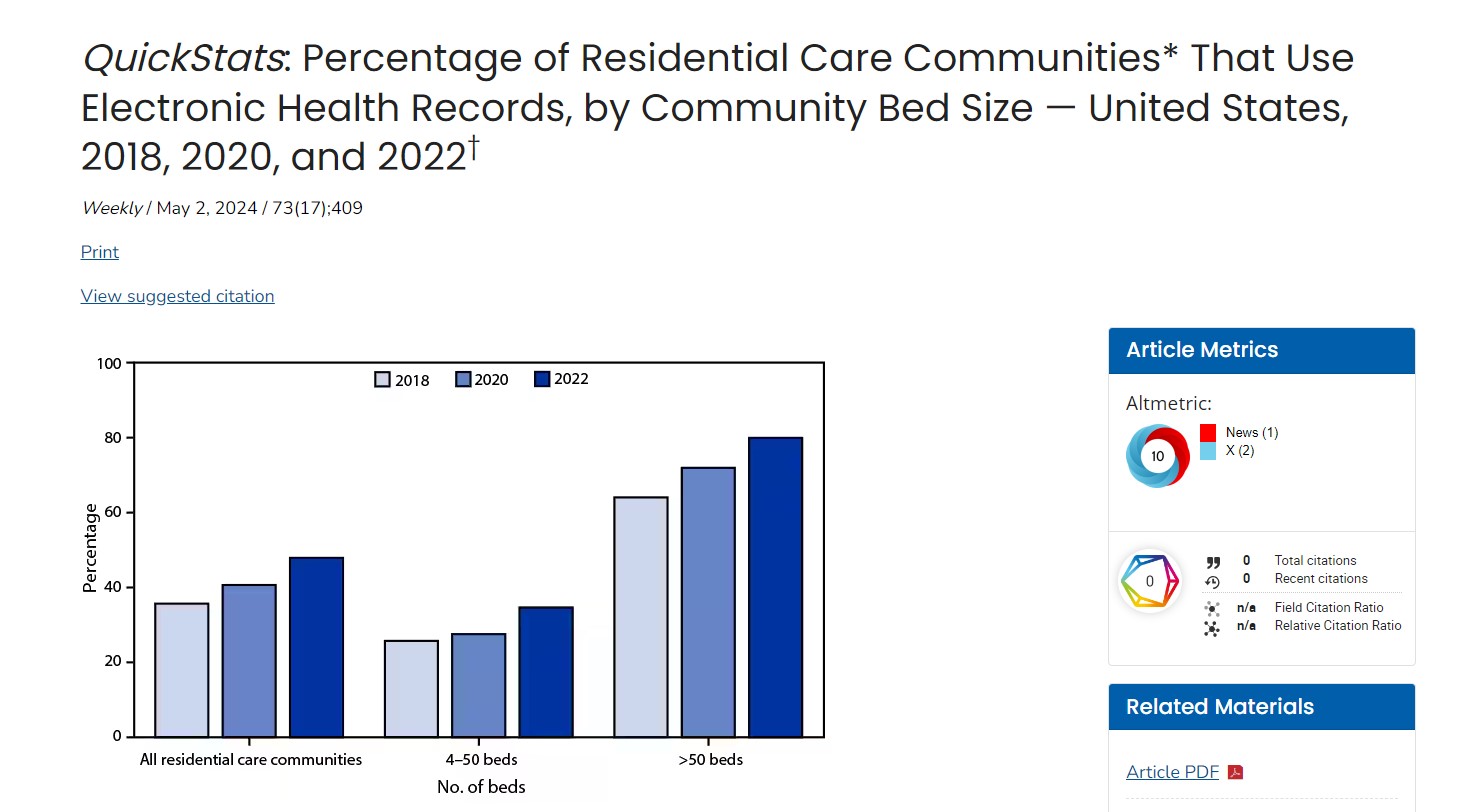
CDC QuickStats: Percentage of Residential Care Communities That Use Electronic Health Records
Evacuation and Health Care Outcomes Among Assisted Living Residents After Hurricane Irma
WHAT THIS MEANS FOR YOU: Using 2017 Medicare data, researchers compared health outcomes from over 25,000 Florida AL residents who resided in an AL on the day of Hurricane Irma’s landfall and either sheltered in place (86% of residents) or evacuated (14% of residents). Evacuation was statistically significantly associated with a 16% higher risk of emergency department visits and with a 51% higher risk of nursing home admissions within 30 days of the hurricane, while hospitalization and mortality rates were similar between the two groups.
Evacuation and Health Care Outcomes Among Assisted Living Residents After Hurricane Irma
WHAT THIS MEANS FOR YOU: Using 2017 Medicare data, researchers compared health outcomes from over 25,000 Florida AL residents who resided in an AL on the day of Hurricane Irma’s landfall and either sheltered in place (86% of residents) or evacuated (14% of residents). Evacuation was statistically significantly associated with a 16% higher risk of emergency department visits and with a 51% higher risk of nursing home admissions within 30 days of the hurricane, while hospitalization and mortality rates were similar between the two groups.
Do-Not-Hospitalize Orders in Assisted Living Facilities: Direct Care Workers’ Perspectives
WHAT THIS MEANS FOR YOU: Eight participants were surveyed and interviewed to inform an intervention that would prevent direct care workers from sending residents with do-not-hospitalize orders to the hospital. Results revealed care workers were unfamiliar with do-not-hospitalize orders and had binary thinking (e.g., residents had to be sent to hospice or the hospital) on end-of-life issues. Supportive leaders in the assisted living communities that could assist direct care workers during these complex situations were found to be helpful.
Do-Not-Hospitalize Orders in Assisted Living Facilities: Direct Care Workers’ Perspectives
WHAT THIS MEANS FOR YOU: Eight participants were surveyed and interviewed to inform an intervention that would prevent direct care workers from sending residents with do-not-hospitalize orders to the hospital. Results revealed care workers were unfamiliar with do-not-hospitalize orders and had binary thinking (e.g., residents had to be sent to hospice or the hospital) on end-of-life issues. Supportive leaders in the assisted living communities that could assist direct care workers during these complex situations were found to be helpful.
Clinical Comorbidities and Transitions Between Care Settings Among Residents of Assisted Living Facilities: A Repeated Cross-Sectional Study
WHAT THIS MEANS FOR YOU: Administrative data from 2013-2019 in Ontario, Canada found a 34% increase in the resident population, and residents experienced increased instances of health conditions including renal disease, mental health issues, cardiac arrhythmias, diabetes, and cancer. Approximately 20% of residents still lived in an assisted living community at the end of the 6-year period, while 10% transitioned to nursing homes. In less than a decade, data revealed increasing medical complexity of assisted living residents, which must be considered for improved policy and practice.
Clinical Comorbidities and Transitions Between Care Settings Among Residents of Assisted Living Facilities: A Repeated Cross-Sectional Study
WHAT THIS MEANS FOR YOU: Administrative data from 2013-2019 in Ontario, Canada found a 34% increase in the resident population, and residents experienced increased instances of health conditions including renal disease, mental health issues, cardiac arrhythmias, diabetes, and cancer. Approximately 20% of residents still lived in an assisted living community at the end of the 6-year period, while 10% transitioned to nursing homes. In less than a decade, data revealed increasing medical complexity of assisted living residents, which must be considered for improved policy and practice.
Hospital Proximity and Emergency Department Use among Assisted Living Residents
WHAT THIS MEANS FOR YOU: This study assessed if the distance between AL communities and the nearest hospital was associated with the frequency of emergency department (ED) visits. Almost 541,000 Medicare beneficiaries aged 55 or older residing in over 16,500 AL communities in 2018-2019 were included. The median distance to the nearest hospital was 2.5 miles. Distance was related to ED use, especially for non-critical, visits, such that communities 5 or more miles from a hospital had fewer ED visits than those that were closer to a hospital.
Hospital Proximity and Emergency Department Use among Assisted Living Residents
WHAT THIS MEANS FOR YOU: This study assessed if the distance between AL communities and the nearest hospital was associated with the frequency of emergency department (ED) visits. Almost 541,000 Medicare beneficiaries aged 55 or older residing in over 16,500 AL communities in 2018-2019 were included. The median distance to the nearest hospital was 2.5 miles. Distance was related to ED use, especially for non-critical, visits, such that communities 5 or more miles from a hospital had fewer ED visits than those that were closer to a hospital.
Injury-Related Emergency Department Use among Assisted Living Residents with Alzheimer’s Disease and Related Dementias
WHAT THIS MEANS FOR YOU: Using 2018 Medicare data for over 116,000 residents, residents with dementia had a 25% higher risk of going to the emergency room for injuries compared to those without dementia, as well as having a significantly higher chance of being hospitalized for injuries, regardless of whether they lived in general assisted living or memory care.
Injury-Related Emergency Department Use among Assisted Living Residents with Alzheimer’s Disease and Related Dementias
WHAT THIS MEANS FOR YOU: Using 2018 Medicare data for over 116,000 residents, residents with dementia had a 25% higher risk of going to the emergency room for injuries compared to those without dementia, as well as having a significantly higher chance of being hospitalized for injuries, regardless of whether they lived in general assisted living or memory care.
Recommendations for Medical and Mental Health Care in Assisted Living Based on an Expert Delphi Consensus Panel
Importance: Assisted living (AL) is the largest provider of residential long-term care in the US, and the morbidity of AL residents has been rising. However, AL is not a health care setting, and concern has been growing about residents’ medical and mental health needs. No guidance exists to inform this care. Objective: To identify consensus […]
Recommendations for Medical and Mental Health Care in Assisted Living Based on an Expert Delphi Consensus Panel
Importance: Assisted living (AL) is the largest provider of residential long-term care in the US, and the morbidity of AL residents has been rising. However, AL is not a health care setting, and concern has been growing about residents’ medical and mental health needs. No guidance exists to inform this care. Objective: To identify consensus […]
Health Care Use and Outcomes in Assisted Living Communities: Race, Ethnicity, and Dual Eligibility
WHAT THIS MEANS FOR YOU: Using Medicare data from 2018, data from over 255,000 people across 24,000 assisted living communities found differences in health outcomes based on race/ethnicity and dual eligibility, including hospital admissions, emergency room (ER) visits, and nursing home placements. For instance, Black and Hispanic residents had lower proportions of ER visits than their white counterparts, but Hispanic residents had higher 30-day readmission rates. Dual eligibility negatively impacted these outcomes more than race/ethnicity alone.
Health Care Use and Outcomes in Assisted Living Communities: Race, Ethnicity, and Dual Eligibility
WHAT THIS MEANS FOR YOU: Using Medicare data from 2018, data from over 255,000 people across 24,000 assisted living communities found differences in health outcomes based on race/ethnicity and dual eligibility, including hospital admissions, emergency room (ER) visits, and nursing home placements. For instance, Black and Hispanic residents had lower proportions of ER visits than their white counterparts, but Hispanic residents had higher 30-day readmission rates. Dual eligibility negatively impacted these outcomes more than race/ethnicity alone.
Impact of Dentures on Oral Health-Related Quality of Life in Assisted Living Facility Elders, Guntur District, Andhra Pradesh
WHAT THIS MEANS FOR YOU: This study investigated how wearing dentures affects the oral health-related quality of life and wellbeing of older adults residing in assisted living in India. Among 587 residents, those using removable partial dentures were more satisfied with their appearance and dental function than those with complete dentures. However, oral health impact (e.g., functional limitations, physical pain, social disability) was higher for complete denture users.
Impact of Dentures on Oral Health-Related Quality of Life in Assisted Living Facility Elders, Guntur District, Andhra Pradesh
WHAT THIS MEANS FOR YOU: This study investigated how wearing dentures affects the oral health-related quality of life and wellbeing of older adults residing in assisted living in India. Among 587 residents, those using removable partial dentures were more satisfied with their appearance and dental function than those with complete dentures. However, oral health impact (e.g., functional limitations, physical pain, social disability) was higher for complete denture users.
Bridging the Transition to Assisted Living: A Framework for Faith Community Nursing
WHAT THIS MEANS FOR YOU: Using an example of an 85-year-old resident, the article proposes a framework for faith community nursing, emphasizing observation, meaningful conversations, advocacy, and assertive communication to ease the move from independent to assisted living.
Bridging the Transition to Assisted Living: A Framework for Faith Community Nursing
WHAT THIS MEANS FOR YOU: Using an example of an 85-year-old resident, the article proposes a framework for faith community nursing, emphasizing observation, meaningful conversations, advocacy, and assertive communication to ease the move from independent to assisted living.
Impact of Function-Focused Care on Psychotropic Medications and Opioid Use among Assisted Living Residents
WHAT THIS MEANS FOR YOU: This study evaluated the impact of function focused care (which trains staff to evaluate residents’ functional capacity and physical activity to optimize their participation in activities) on the use of psychotropic medications and opioids. The study observed 794 residents across 85 communities over 12 months. There was a reduction in opioid use in the treatment group after four months; in the full sample during the overall study period, there was an increase in the use of benzodiazepines and antipsychotics.
Impact of Function-Focused Care on Psychotropic Medications and Opioid Use among Assisted Living Residents
WHAT THIS MEANS FOR YOU: This study evaluated the impact of function focused care (which trains staff to evaluate residents’ functional capacity and physical activity to optimize their participation in activities) on the use of psychotropic medications and opioids. The study observed 794 residents across 85 communities over 12 months. There was a reduction in opioid use in the treatment group after four months; in the full sample during the overall study period, there was an increase in the use of benzodiazepines and antipsychotics.
Potential Side Effects and Adverse Events of Antipsychotic Use for Residents With Dementia in Assisted Living: Implications for Prescribers, Staff, and Families
WHAT THIS MEANS FOR YOU: This study examined the use of antipsychotic medications among residents with dementia in 91 AL communities across seven states. The prevalence of potential side effects was high (93%) and of possible adverse events low, (6%), potentially associated with medication side effects. Quetiapine (Seroquel) and risperidone (Risperdal) were the most frequently prescribed antipsychotics. Most, but not all, residents’ family members were aware of their relative’s antipsychotic use.
Potential Side Effects and Adverse Events of Antipsychotic Use for Residents With Dementia in Assisted Living: Implications for Prescribers, Staff, and Families
WHAT THIS MEANS FOR YOU: This study examined the use of antipsychotic medications among residents with dementia in 91 AL communities across seven states. The prevalence of potential side effects was high (93%) and of possible adverse events low, (6%), potentially associated with medication side effects. Quetiapine (Seroquel) and risperidone (Risperdal) were the most frequently prescribed antipsychotics. Most, but not all, residents’ family members were aware of their relative’s antipsychotic use.
Rapid Adoption of Electronic Health Record and Health Information Exchange among Assisted Living Communities, 2010–2018
WHAT THIS MEANS FOR YOU: This study examined the use of electronic health records (EHRs) and health information exchange (HIE) in AL between 2010 and 2018. Use varied based on AL size and ownership, with larger (26+ beds) and chain-owned communities more likely to use these technologies. Overall, adoption of these technologies increased from 2010 to 2018, but smaller communities had lower adoption rates.
Rapid Adoption of Electronic Health Record and Health Information Exchange among Assisted Living Communities, 2010–2018
WHAT THIS MEANS FOR YOU: This study examined the use of electronic health records (EHRs) and health information exchange (HIE) in AL between 2010 and 2018. Use varied based on AL size and ownership, with larger (26+ beds) and chain-owned communities more likely to use these technologies. Overall, adoption of these technologies increased from 2010 to 2018, but smaller communities had lower adoption rates.
Reimagining Medical Care in Assisted Living
WHAT THIS MEANS FOR YOU: Three industry-wide proposals were recommended to enhance medical care quality for AL residents: regular on-site medical visits; employing experienced professionals in long-term and end-of-life care; and the introduction of an AL medical director role to establish rules, staff qualifications, and collaboration. The researchers acknowledge that adaptations may be necessary to adhere to these recommendations due to community size and availability of resources.
Reimagining Medical Care in Assisted Living
WHAT THIS MEANS FOR YOU: Three industry-wide proposals were recommended to enhance medical care quality for AL residents: regular on-site medical visits; employing experienced professionals in long-term and end-of-life care; and the introduction of an AL medical director role to establish rules, staff qualifications, and collaboration. The researchers acknowledge that adaptations may be necessary to adhere to these recommendations due to community size and availability of resources.
Model Testing of the Factors that Influence Performance of Function Focused Care and Function among Assisted Living Residents
WHAT THIS MEANS FOR YOU: A study of 550 AL residents from 59 communities found that factors such as better physical and cognitive health, positive care interactions, and supportive environments were associated with increased participation in function-focused care. Additionally, for-profit communities had higher levels of function-focused care despite having residents with lower functioning.
Model Testing of the Factors that Influence Performance of Function Focused Care and Function among Assisted Living Residents
WHAT THIS MEANS FOR YOU: A study of 550 AL residents from 59 communities found that factors such as better physical and cognitive health, positive care interactions, and supportive environments were associated with increased participation in function-focused care. Additionally, for-profit communities had higher levels of function-focused care despite having residents with lower functioning.
The Impact of Cognitive Impairment on Clinical Symptoms, Physical Activity and Care Interactions among Residents in Assisted Living Settings
WHAT THIS MEANS FOR YOU: This study included 550 AL residents from 59 communities, and assessed how cognitive impairment relates to physical activity, pain, and willingness to receive staff-assisted function-focused care. It found that cognitively impaired residents were less active, experienced more pain, and were less interested in staff-assisted function-focused care activities.
The Impact of Cognitive Impairment on Clinical Symptoms, Physical Activity and Care Interactions among Residents in Assisted Living Settings
WHAT THIS MEANS FOR YOU: This study included 550 AL residents from 59 communities, and assessed how cognitive impairment relates to physical activity, pain, and willingness to receive staff-assisted function-focused care. It found that cognitively impaired residents were less active, experienced more pain, and were less interested in staff-assisted function-focused care activities.
Post-Acute Care Transitions and Outcomes among Medicare Beneficiaries in Assisted Living Communities
WHAT THIS MEANS FOR YOU: Medicare data were used to analyze post-acute care referrals for over 104,000 assisted living residents. The most common referral after hospitalizations was to skilled nursing. Referrals to skilled nursing were associated with a lower likelihood of emergency department visits and hospital readmissions; however, there was higher likelihood of long-term skilled nursing placement and death.
Post-Acute Care Transitions and Outcomes among Medicare Beneficiaries in Assisted Living Communities
WHAT THIS MEANS FOR YOU: Medicare data were used to analyze post-acute care referrals for over 104,000 assisted living residents. The most common referral after hospitalizations was to skilled nursing. Referrals to skilled nursing were associated with a lower likelihood of emergency department visits and hospital readmissions; however, there was higher likelihood of long-term skilled nursing placement and death.